[ad_1]
While type 2 diabetes is largely preventable, type 1 diabetes is a disruptive autoimmune disorder that was one time incurable thinking. “Once” is the key word here, as a new and uncontroversial form of stem cell treatment should be able to cure the disease once and for all.
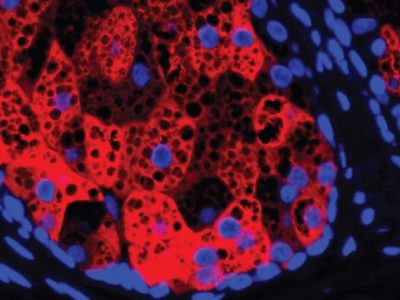
The treatment, which is based on transforming a small portion of adult skin tissue into beta cells in the pancreas, which produce the illusory hormone insulin in diabetics, prevents the genetic mutation that causes the immune system to attack these cells that create the disease .
Diabetes, especially type 1, severely limits quality of life and, if not managed carefully, can lead to serious complications such as foot amputations and early mortality.
Plus, it costs the US healthcare industry. about $ 85,000 per patient over a lifetime, a huge burden that, if removed, could save the entire industry hundreds of millions.
Researchers at the Salk Institute for Biological Studies, a leading force in all forms of biology, have pioneer in a new way to produce pancreatic beta cells for this type 1 treatment, and now the only thing keeping it from being available in a hospital is human safety trials.
“Stem cells are an extremely promising approach to develop many cell therapies, including better treatments for type 1 diabetes,” said Salk professor Juan Carlos Izpisua Belmonte, lead author of the corresponding paper, he told Salk’s press department.
“This method of making large numbers of safe and functional beta cells is an important step forward.”
The reason the stipulation is important is that while your article mentions 11 citations on the concept of using stem cell therapy to cure diabetes, since 2007, there are challenges, yet to be overcome, with manufacturing beta cells. of the pancreas.
Growing a cure
Before stem cells were used, patients could receive transplanted islet cells of donors with a fully functional insulin system, but low donor rates made this treatment slow, even though it was successful.
Existing stem cell methods only successfully convert about 10-40% of human pluripotent stem cells (PSCs) into beta cells of the pancreas. In addition, pancreatic beta cells of PSCs tend to be heterogeneous and contain unwanted cell types that can impede or disrupt the maturation and function of the desired pancreatic beta cells.
Previous methods Using PSC to create beta cells also sometimes results in dysfunction or, in some cases, the formation of teratomas (sometimes huge) or cysts.
“For beta cell-based treatments to eventually become a viable option for patients, it is important to make these cells easier to manufacture,” co-lead author Haisong Liu, a former member of Dr. Belmonte. “We need to find a way to optimize the process.”
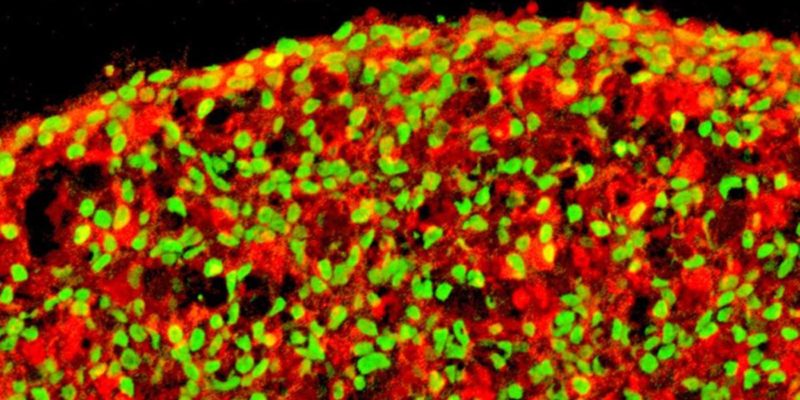
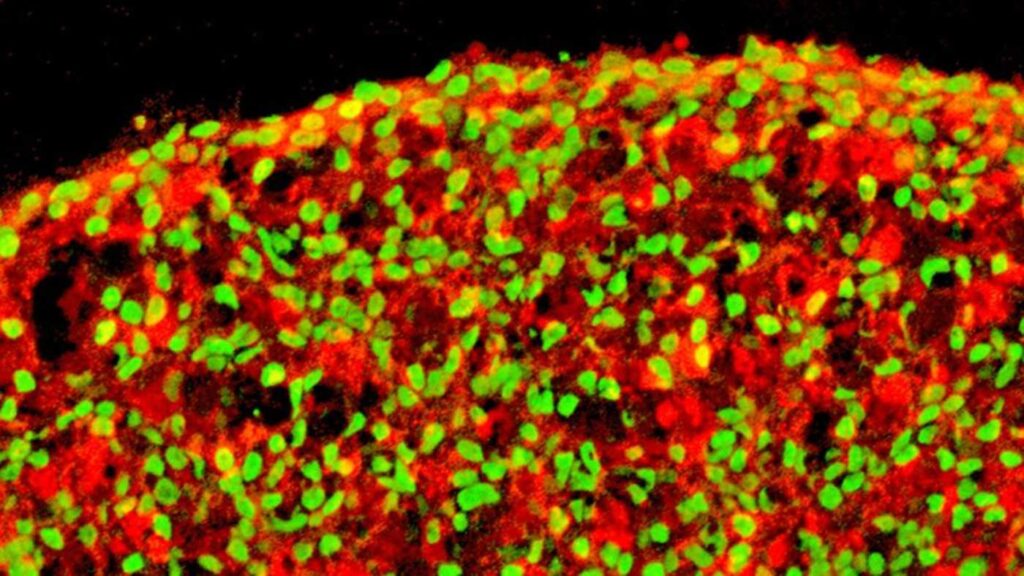
And they did just that. The use of a three-dimensional Petri dish allowed the cells to interact and grow in an environment similar to what they would naturally do, and within two weeks of transplantation into diabetic mice, their blood sugar levels dropped to normal levels. as observed in non-diabetic mice.
RELATED: Walmart Introduces Low-Price Insulin for Diabetes Patients Who Can’t Afford It Easily
To test the safety and efficacy of the manufactured beta cells, the team transplanted them at different stages and observed the effects. At the highest stages of growth, cells did not result in cyst formation even 20 weeks after implantation and exhibited adequate functionality. live Y in vitro.
The three-dimensional stem cell production method will continue to be refined at Salk, with the only hurdled human trials remaining and FDA approval. At least one pharmaceutical company has already shipped this year in trials to test stem cell therapy for type 1 diabetes, so it seems the days of the medical condition are numbered.
SHARE this hopeful investigation with friends on social media …
[ad_2]
Original source