[ad_1]
Scientists confirm that mothers and children share a biological connection known as maternal-fetal microchimerism. This means that cells from a developing baby travel to the mother’s bloodstream and circulate back to the baby. The term microchimerism comes from the word chimera, mythical creatures made from various animals in ancient Greek mythology.
In biology, it means “an organism that contains a mixture of genetically different tissues.” In a way, we are all chimeras since our DNA comes from both our mothers and our fathers.
We know that pregnant mothers pass nutrients and DNA through the placenta to their unborn children. However, scientists have also found a child’s genetic material in mothers long after pregnancy, even decades later.
The evidence scientists discovered
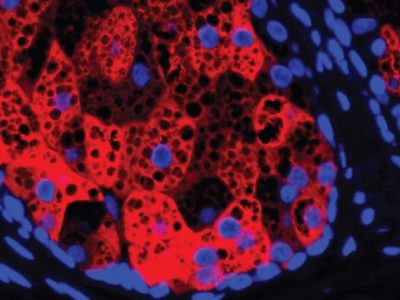
Scientists have found evidence that all pregnant women possess some of the fetal cells and DNA of their children. In fact, up to 6% of the free-floating DNA in the mother’s blood plasma comes from the fetus. Although these numbers decrease after the baby is born, some cells remain in the mother. In the 1990s, a team of researchers at Tufts Medical Center found male fetal cells in the mother’s blood 27 years postpartum.
These fetal cells can act as stem cells, transforming into different types of cells to help repair damage to their mothers’ organs. Cells can influence a mother’s long-term health and explain why previous pregnancy can protect women against diseases such as breast cancer.
This suggests that even before birth, babies have an innate instinct to survive. By taking care of your mother’s health, you ensure that the baby can develop safely. Fetal microchimerism also helps the mother heal from life-threatening illnesses. Scientists have discovered that stem cells can develop into epithelial cells, specialized heart cells, liver cells, and even neurons.
However, although fetal cells can improve the health of the mother, a 2015 study found that Microchimerism can also affects negatively. Researchers at Arizona State University found that cells could act cooperatively or competitively, depending on the circumstances. They have been linked to protection and an increased risk of many diseases, such as cancer and autoimmune disorders.
How Fetal Microchimerism Affects Maternal Health
This phenomenon can be found in all mammalian species, such as dogs, mice, and cows. Scientists are just beginning to understand this alien concept and how it affects both mother and baby. When ASU scientists reviewed published studies on fetal microchimerism, they discovered the true complexity of fetal cells.
For the study, they applied an evolutionary framework to predict the behavior of fetal cells. This would help them understand when the cells benefited the mother and caused adverse effects. They found that fetal cells don’t just migrate to maternal tissues; they also act as a placenta outside the uterus. Cells redirect essential nutrients and genetic material from the mother to the developing fetus.
How does it work
In short, there is a constant tug of war between the interests of the mother and the child. There is also a mutual desire to survive, which requires cooperation between the baby and the mother. The mother passes vital nutrients to her baby and the fetus passes DNA into the maternal system.
If fetal microchimerism benefits the survival of the mother and the offspring in most cases, it will become part of the evolutionary adaptation. Review of existing data found that fetal cells have a cooperative relationship with maternal tissues in some cases. In other cases, fetal cells compete for resources or may exist as neutral entities. Scientists believe that cells are likely to play all of these roles in various situations.
For example, fetal cells can elicit immune responses and even autoimmunity if the mother recognizes them as foreign bodies. They may explain the increased rates of autoimmunity in women. For instance, rheumatoid arthritis it occurs three times more often in women than in men.
Fetal microchimerism can also benefit the mother, even helping to heal wounds from cesarean incisions. This shows that fetal cells play an active role in the repair of the mother’s tissues. However, the cells can also enter the mother’s bloodstream and act as bystanders, without helping or harming the mother.
The complex nature of fetal microchimerism.
The authors used a cooperative and conflict approach to help predict the positive or negative influence of fetal cells on mothers. This gave them more insight into the circumstances that cause cells to cooperate or compete for resources.
According to evolutionary theory, fetal cells will cooperate when the cost does not outweigh the risk, such as tissue maintenance. However, competition is the likely outcome in situations where limited resources must be allocated between the fetus and the mother. This conflict can have harmful effects on both mother and baby.
The researchers looked at the tug of war in fetal cells in female breasts, for example. The cells have been detected in the breasts of more than half of the women sampled. Fetal microchimerism plays an active role in breast development and lactation. While the production of milk ensures the survival of the baby, it also requires a lot of energy from the mother.
Scientists have found that poor breastfeeding, a common occurrence, may be due to a low fetal cell count in breast tissue. Breast milk fetal count testing could provide concrete evidence of the impact of fetal cells on maternal health.
The relationship between breast cancer and fetal cells is also a complicated matter. The scientists found that women with breast cancer tend to have a lower fetal cell count. However, some data shows that fetal cells can increase the risk of breast cancer for several years after a woman gives birth.
Finally, fetal cells can also affect a woman’s thyroid function. Fetal cells have been found more frequently in the blood and thyroid glands of women with thyroid diseases, including Hashimoto’s disease, Graves’ disease, and thyroid cancer. The study authors believe that a woman’s immune system can be over-activated by controlling the influence of fetal cells. This could lead to high levels of autoimmunity and inflammation, contributing to autoimmune disease.
Final thoughts: fetal cells affect the health of the mother during pregnancy and beyond
Fetal cells can travel to the mother’s bloodstream and return to the baby, also known as fetal-maternal microchimerism. This phenomenon has been observed in all placental mammals. However, scientists are just beginning to unravel the complicated relationship between a mother and her developing fetus.
It is clear that researchers will need to continue studying fetal microchimerism, as it is a very complex subject. They hope that future studies will lead to improvements in diagnosing conditions and predicting long-term maternal health.
[ad_2]
Source link here